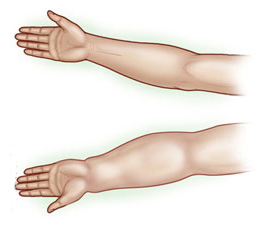
The lymphatic system collects lymph fluid (excess fluid, proteins, and other substances) from the body tissues and carries it back to the bloodstream. Lymph fluid moves slowly through lymphatic vessels and passes through lymph nodes as it returns to the bloodstream. Swelling occurs when the normal drainage of fluid is disrupted, and lymph fluid accumulates in the body tissues. This can be due to a blockage or surgical removal of lymph nodes. This results in large amounts of lymph fluid collecting in the tissue.

Lymphedema can be a hereditary condition. Most often, however, it results from blockages in lymph vessels caused by infection, cancer, and scar tissue due to radiation therapy or the surgical removal of lymph nodes.
You are at greater risk for lymphedema if you:
- Had surgery to remove your lymph nodes in the underarm, groin, or pelvic area.
- Received radiation therapy to your underarm, groin, pelvic region, or neck.
- Have scar tissue in the lymphatic ducts, veins, or under the collarbones, caused by surgery or radiation therapy.
- Received taxane chemotherapy.
- Have cancer that has spread to the lymph nodes in the neck, chest, underarm, pelvis, or abdomen.
- Have tumors in the pelvis, abdomen, or chest that put pressure on your lymphatic vessels and/or lymphatic duct and block fluid drainage.
- Have inflammation of the arm or leg after surgery.
- Are older.
- Have a poor diet or are overweight. These conditions may delay recovery from surgery and radiation therapy and increase the risk of lymphedema.
Signs and Symptoms
With lymphedema, you may have:
- Swelling in your arms, legs, shoulders, hands, fingers, chest, or neck.
- Skin that feels tighter, harder, or thicker than normal in the affected area.
- Aching, tingling, or a feeling that your arm or leg is heavy.
- Weakness in your arm or leg.
- Inability to move certain joints, such as your wrist or ankle, as freely as usual.
- Pitting (indentation) in the tissues of your limb (made by pressing a finger on the skin that takes time to “fill in” after removing the pressure).
- Clothing, rings, bracelets, or shoes that fit tighter than before.
- Repeated infections in your arm or leg.
- Joint pain.
- Difficulty doing your daily activities.
If you have fever and chills, and your limb with lymphedema is red, swollen, or painful and feels warm to the touch, you may have an infection. Contact your doctor.
How Is It Diagnosed?
Your physical therapist will review your medical history and medicines and perform a thorough physical examination. They also will gather the following information:
- Your actual weight compared with your ideal weight.
- Circumference measurements of your arms, legs, chest, and neck.
- How well you’re able to do activities of daily living. These include bathing and grooming, dressing and undressing, or walking, eating, and drinking.
- Whether you have a history of edema, radiation therapy, chemotherapy treatments, or surgery.
- The amount of time between surgery and when you first noticed the swelling in a limb.
- A history of other chronic health conditions such as diabetes, high blood pressure, kidney disease, heart disease, or phlebitis (inflammation of the veins).
How Can a Physical Therapist Help?
Your physical therapist will serve as an important member of your health care team. They will work closely with you to design a treatment program to help control the swelling and meet your goals for returning to your activities.
In the early stages of lymphedema, when the swelling is mild, it often can be managed by techniques that encourage lymph flow such as:
- Compression garments.
- Exercise.
- Elevation of the affected limb.
For more severe swelling, your physical therapist may use a treatment plan called complete decongestive therapy to help improve the flow of lymph fluid. This includes:
- Manual lymphatic drainage, which feels like a light form of massage.
- A personalized exercise program.
- Compression bandaging to help reduce your swelling.
- Providing you with information on skin and nail hygiene to reduce the risk of infection.
Your physical therapist will carefully monitor the size of your affected limb throughout your treatment sessions. Once the size of your limb has decreased to the desired measurements, your physical therapist will help you begin to take over your own care and will:
- Develop a safe and sensible personalized exercise program for you to do on your own. This program will help you increase your physical fitness without overly straining your affected arm or leg.
- Update your compression garments to ensure they fit properly and best meet your needs.
- Educate you about how proper nutrition and diet, and skin and nail care can help reduce your risk of infection.
Can This Injury or Condition Be Prevented?
Some risk factors for lymphedema, such as treatment for cancer, cannot be avoided. If you have had your lymph nodes removed, or received radiation or certain chemotherapies, but you don’t have lymphedema, you might still be at risk for developing it. Your physical therapist will help you identify factors that may increase your risk for lymphedema. They will provide you with suggestions for managing these risks so that you can reduce the likelihood of developing it.
Your physical therapist will:
- Design a safe and sensible individualized home exercise program to improve your overall fitness and help you avoid a weight gain that can increase your risk of lymphedema.
- Develop a safe and sensible exercise program that will avoid straining the affected limb and help you reduce the risk of developing lymphedema following surgery or infection.
- Periodically assess the size of your limb and, if there is an increase in limb size, provide conservative, early intervention to help prevent further swelling.
- Help you maintain good skin/nail care and hygiene.
Poor drainage of the lymphatic system might make infection of your arm or leg more likely. Even a small infection could lead to serious lymphedema. You can help prevent infections from occurring by avoiding cuts and abrasions, burns, punctures, and insect bites on your affected limb.
_____________